Insulin Treatment of Type I Diabetes
Normal Insulin Production
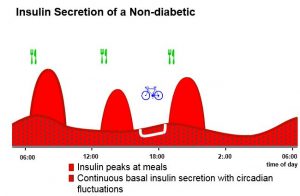
In non-diabetic people, insulin is automatically released from the pancreas in response to a rise in blood glucose following a meal. This allows the glucose to be taken up by the body’s cells where it is either used straight away, or stored (mostly in the liver or muscles) for later. So, in the presence of insulin, glucose is removed from the blood and the blood glucose level drops again. Just the right amount of insulin is produced to keep the blood glucose level within normal limits. In addition to this, small amounts of insulin are continuously produced between meals and overnight, in order to keep the body ticking over.
Insulin Therapy for People with Type 1 Diabetes
People with Type 1 diabetes produce no insulin and therefore depend on insulin injections to stay alive. (People with Type 2 diabetes usually produce some insulin and many are treated with diet and tablets that enable them to make better use of the insulin that they produce.) The aim of diabetes management is to keep blood glucose levels close to normal. For those people who require insulin, this means coordinating insulin injections with meals and snacks, whilst counterbalancing the effects of activity levels.
There are a number of ways in which insulin is used to treat people with diabetes:-
- Conventional Therapy
- Intensive Therapy
- Insulin Pump Therapy (also known as continuous subcutaneous insulin infusion or CSII)
Conventional Therapy
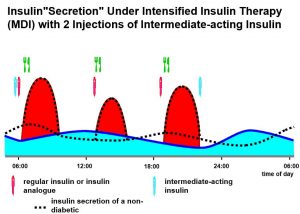
Conventional therapy usually consists of two insulin injections a day. Each injection contains some short acting insulin and some intermediate or long acting insulin. In theory, short acting insulin at breakfast supplies insulin for the morning and long acting insulin at breakfast supplies insulin for the afternoon. Then, short acting insulin in the early evening supplies insulin for that evening and long acting insulin in the early evening supplies insulin for overnight. Separate doses of short and long acting insulin can be drawn up together into the same syringe. Alternatively, a number of ready mixed insulins are available that contain short and long acting insulin in fixed proportions. Conventional therapy offers the advantage of not having to inject at lunchtime and some people may see this as a bonus. However, the major drawback of conventional therapy is the lack of flexibility; timing of meals is dictated by the injection routine. Also, if pre-mixed insulins are used, there is no room for altering the dosage of short or long acting insulin independently from the other – another mixture needs to be used. In addition, the insulin injections tend not to match the body’s natural daily needs for insulin.
Intensive Therapy
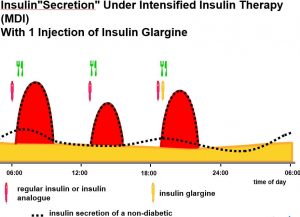
Intensive therapy usually involves Multiple Daily Injections (i.e. 3 or more) of insulin (and is sometimes referred to as ‘MDI’). Long acting insulin (e.g. Isophane or Glargine) is given once (or sometimes twice) daily and quick acting insulin is given before each meal. In theory, the long acting insulin supplies the body’s background needs, whilst the short acting insulin ‘covers’ meals. This type of injection regimen aims to provide a more natural supply of insulin supply and increases flexibility in terms of mealtimes. However, the long acting insulin often fails to provide the appropriate ‘background’ insulin needs leading to erratic swings in blood sugar levels.
Insulin Pump Therapy
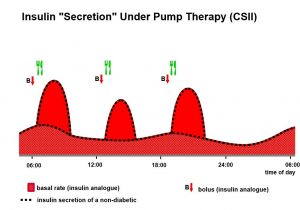
Rather than injecting the insulin, it can be supplied by a small pump, which is worn all the time. The insulin is delivered to the body through a fine tube with a needle or cannula that sits under the skin. The pump mimics the function of the pancreas in that it provides a steady supply of ‘background’ or basal insulin and extra spurts or bolus doses of insulin are given before eating. The basal supply of insulin through the day can be altered so that it is in tune with your own body’s individual needs. The basal insulin keeps the blood glucose levels stable in-between meals and overnight. The bolus doses are specifically tailored to food intake. With Insulin Pump Therapy there is no need to plan meals and activities around insulin injections. Although the pump does not measure blood glucose levels and produce insulin automatically – you have to test your own blood glucose and program the pump yourself – Insulin Pump Therapy is the most natural form of insulin treatment available today.
Insulin Pump Therapy is also known as continuous subcutaneous insulin infusion (CSII).